
|

|
|
 Clinical Forensic Medicine - A Physician's Guide, 2ndEdition, Edited by Margaret M. Stark. Hard Bound, 6" x 9". [Includes eBook/PDA on CD-ROM]. Foreword by Sir John Stevens, former Commissioner of the Metropolitan Police Service, London, UK
Clinical Forensic Medicine - A Physician's Guide, 2ndEdition, Edited by Margaret M. Stark. Hard Bound, 6" x 9". [Includes eBook/PDA on CD-ROM]. Foreword by Sir John Stevens, former Commissioner of the Metropolitan Police Service, London, UK
Humana Press Inc., 999 Riverview Drive, Suite 208, Totowa, New Jersey 07512; Publication Date: 11 April 2005. xvii + 438 pages, ISBN 1-58829-368-8, E-ISBN 1-59259-913-3. List price US $99.50 (10% discount with online order).
 Amazon Link: Click here to visit
Amazon Link: Click here to visit
 |
This is such a revolutionary book, we thought we should give some excerpts from it, to enable the reader to gauge a better idea about its excellence.
One of the most useful chapters in the book is on Injury assessment, documentation and interpretation (chapter 4) written by Jason Payne-James, Jack Crane and Judith A. Hinchliffe. The figures throughout the book are in black and white, but the accompanying CD gives several of these figures in color. We are reproducing the color photographs in the following excerpt. The authors are talking about evidence collection in cases of injury [pages 154-8].
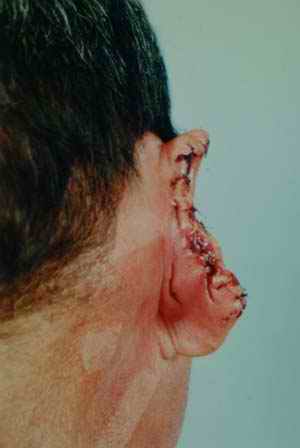
As soon as it has been established that the injury has been caused by biting, the injury should be photographed and swabbed for saliva. In addition, it may be necessary to take an impression of the injured site to preserve any possible indentations. Clearly, the taking of forensic samples is not always possible when the injured party needs urgent medical attention. Often, the forensic dentist is provided with photographs taken some time after the incident date and after medical intervention (see Fig. 12); by this time dental evidence has been lost, but it may still be possible to identify the injury as a possible biting injury.
Saliva is deposited on the skin (and clothing, if present) during biting and sucking. The quantity and quality of this may enable DNA analysis after swabbing of the unwashed injury site. The double-swab technique is effective for this procedure (12). Please note that salivary DNA has been reported as having been recovered from the bitten breast of a young deceased woman found submerged in water (13). The saliva swabs (with controls) must be clearly and correctly labeled and stored appropriately (see Chapter 3).
Oral saliva samples will be needed from any potential suspect, and the victim of an assault if there is a possibility that the victim bit the assailant (or self-infliction is suspected).
 |
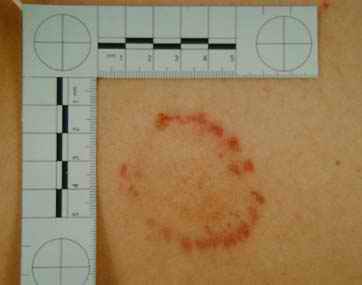
Photographs should be taken when the bite mark is first discovered. It is essential for correct photographic procedures to be followed to minimize distortions. Police photographers experienced in crime scene and other injury photography may still find the assistance of the forensic dentist useful, because complications arise from curved surfaces and the correct positioning of the camera and scales. The American Board of Forensic Odontology no. 2 scale, being small and "L" shaped, is very effective (14) and is now used by many police forces.
Skin is not the best impression material, and various papers and reports have shown the importance of photographing the victim in the same position as when bitten in an attempt to minimize distortion (15,16). However, this is not always possible. Changes in the injury with time (in both the living and the deceased) may mean that the injury pattern appears clearer after a day or two. There is no reliable way of knowing when an injury will reveal the most detail, and, therefore, repeat photography (e.g., every 24 hours for 3-5 days) can prove useful.
Ultimately, the forensic dentist will select the best photographs and have them reproduced to life-size (1:1) for analysis and comparison work. At the time of writing, conventional film photography is still widely used, but the use of digital photography is progressing rapidly. Whatever the future brings, it is essential that standards, protocols, and appropriate training are in place.
 |
Dental impressions taken from the potential biter by the dentist (or appropriately qualified person) after a thorough dental examination will be cast into hard dental models. Dental impressions taken of an individual in custody are intimate samples and require the appropriate authority and consent for your jurisdiction. Transparent overlays of the biting edges of the teeth from the dental models will be produced to facilitate physical comparisons. Currently, the best method for overlay production to achieve accuracy and reproducibility is the computer-generated method (17).
The importance of following the correct procedures for evidence documentation, collection, preservation, and storage with continuity of evidence cannot be overstressed.
The biting injury demonstrating plenty of detail (see Fig. 13) that has been carefully examined, recorded, analyzed, and interpreted can be useful to the justice system. It can establish contact between two people or, of equal importance, exclude an innocent party. Early suspicion and recognition by personnel involved with the investigation, followed by prompt and appropriate action, will help maximize the opportunity to collect evidence. Awareness by all concerned and early referral to the forensically trained dentist with experience in this field promote teamwork and best practice.
In chapter 6 entitled "Crowd-control agents", author Kari Blaho-Owens gives a fascinating account of various crowd control agents. Here is what the chapter says on Oleum capsicum [pages 182-7].
OC selectively stimulates nociceptors in exposed mucous membranes, releasing substance P, bradykinin, histamine, and prostaglandins. The physiological effects of these mediators' results in vasodilation, increased vascular permeability, pain, and altered neurotrophic chemotaxis. Other common symptoms are listed in Table 2.
Finding |
Chlorobenzylidene |
Chloracetothenon |
Capsaicin oleum |
Ocular |
|
|
|
• Lacrimation |
|
|
|
• Blepharospasm |
|
|
|
• Pain and/or burning at exposure site |
|
|
|
• Conjunctival injection |
|
|
|
• Conjunctival edema |
|
|
|
• Photophobia |
|
|
|
• Corneal abrasion |
|
|
|
• Impaired vision |
|
|
|
|
|
|
|
Upper airway |
|
|
|
• Pain and/or burning |
|
|
|
• Shortness of breath |
|
|
|
• Increased secretion |
|
|
|
• Congestion |
|
|
|
• Coughing |
|
|
|
• Throat irritation |
|
|
|
• Wheezing |
|
|
|
• Irregular respiration a |
|
|
|
|
|
|
|
Dermal |
|
|
|
• Pain |
|
|
|
• Contact dermatitis |
|
|
|
• Blistering |
|
|
|
|
|
|
|
Miscellaneous |
|
|
|
• Nausea/vomiting |
|
|
|
• Bad taste |
|
|
|
• Headache |
|
|
|
• Increased blood pressure |
|
|
|
a Initial response believed to be associated with pain.
Capsicum in its pure form is a crystalline material. The oleoresin extract of capsicum contains more than 100 volatile compounds that act similarly to capsicum (16). Because of the variability in the individual components of OC, the relative pungency of the pepper type and geographical origin of the pepper, and variation in quality control, products containing this extract have differences in efficacy (16,17). Commercially available OC products lack standardization for capsaicinoid content, which may alter potency, ultimately lead to variability in its efficacy, and jeopardize the safety of the user because of lack of effect (18). Most OC preparations are formulated in a propylene vehicle to enhance adherence to the skin surface. PS is the most common spray marketed to civilians for a less lethal, noncontact, self-defense method. It can be purchased in numerous sprays or foams, in various concentrations, or combined with other crowd-control agents, such as CS (see Fig. 1).
 |
In a retrospective study by Watson et al. (8), patients presenting to an emergency department (ED) after PS exposure during a law enforcement action were evaluated. Most patients complained of ocular irritation and irritation and pain at the exposure site. The symptoms were transient, and few required treatment. The most significant adverse effects were corneal abrasions, which were treated with topical anesthetics and topical antibiotics. Five of 94 patients complained of wheezing or shortness of breath. No patient required treatment for wheezing, and two of the five had a history of reactive airway disease. No patient in this study had significant morbidity or mortality, and all were discharged from the ED. There are no data to support that PS exacerbates pulmonary disease or that patients with reactive airway disease are more sensitive to the effects (8,19-21).
There have been a few reports of severe reactions to PS. One case report summarized respiratory distress that necessitated extracorporeal membrane oxygenation in a 4-wk-old infant after a 5% PS was accidentally discharged in his face (22). The infant had a rocky clinical course but recovered. Another case report summarized the clinical course of an 11-yr-old child who intentionally sprayed and inhaled PS from an individual canister and developed reversible wheezing (23). These case reports are anecdotal in that they report symptoms temporally related to PS exposure and demonstrate that when used improperly these compounds can cause severe symptoms. Thus far, these adverse events have been rare.
Of concern were reports of violent prisoners who died after being sprayed with PS and being physically restrained (24). It was assumed that the police used excessive force and that the prisoners died from "positional asphyxia" from the restraints and that PS played a role in their deaths (24).
 |
 |
The cause of in-custody deaths can be difficult to determine because many times these deaths have other confounding factors besides restraint and chemical control agents. Risk factors for sudden death, such as mental illness, drug abuse, and seizure disorders, may not be readily visible, and autopsy reports can often be inconclusive or incomplete. There is no evidence that PS causes any type of respiratory effects sufficient to cause death, nor is there evidence to conclude that positional asphyxia caused the deaths of those in question. All of the prisoners who died exhibited characteristics consistent with excited delirium from substance abuse. Most were obese, had hyperthermia, were violent, and had measurable cocaine on postmortem analysis. The lesson learned from these cases is that all violent prisoners, regardless of whether a chemical restraint has been used, should be closely monitored and evaluated by appropriate health care professionals. A small population of acutely intoxicated individuals is at risk of sudden death, independent of their treatment.
To refute the association between restraint and OC exposure, Chan et al. performed a randomized, crossover, controlled trial to assess the effect of OC spray inhalation with OC exposure plus restraint in a prone position (25). Results from 35 subjects exposed to OC or placebo showed that inhalation of OC did not result in abnormal spirometry, hypoxemia, or hypoventilation when compared to placebo in either sitting position or in a maximal restraint position.
Treatment of exposure to PS is based on severity of symptoms. The first order of treatment should always be decontamination, which includes actions to limit exposure, such as the removal of contaminated clothing. Copious irrigation of affected areas will attenuate the burning sensation (26,27). However, one must use caution not to contaminate other sites with the irrigant (e.g., washing PS from the hair into the eyes or oral pharyngeal mucosa). In a study, topical proparacaine was helpful in alleviating ocular pain associated with OC exposure (approx 50% of those treated experienced an improvement in their symptons) when compared to a topical nonsteroidal antiinflammatory agent (0.03% topical flurbiprofen) or placebo (28). It is important to note that there were no corneal abrasions in any of the 11 subjects in this study and that 21% of the eyes had slit lamp evidence of punctuate epithelial erosions. In this study, as well as an additional exposure trial, the focal epithelial damage healed within 1 d, independent of treatment (29).
For those with ocular exposure to OC, a slit lamp examination of the anterior chamber is warranted to rule out corneal abrasion in patients who remain symptomatic for more than 30 min. If present, the abrasion should be treated appropriately with topical local anesthetics, topical antibiotics, cycloplegics, analgesics, and follow-up care. Dermatitis associated with PS has been reported (30,31). Topical corticosteroids, systemic antihistamines, and analgesics have been employed in reducing symptoms. An example of rather severe PS dermatitis and ocular swelling is shown in Fig. 2. This particular patient was sprayed during arrest by police officers and brought to an ED for evaluation. He was treated with irrigation, systemic antihistamines, and steroids, with resolution of his symptoms within 4 d.
As would be quite evident to the reader by reading these excerpts, this book is quite useful to all forensic physicians, or any doctor involved in forensic examination of the living. Highly recommended!
 Order Humana Press Books by clicking here.
Order Humana Press Books by clicking here.
or via telephone: (973) 256-1699 or Fax: (973) 256-8341 or Email: humana@humanapr.com
 Request a PDF file of this review by clicking here. (If your screen resolution can not be increased, or if printing this page is giving you problems like overlapping of graphics and/or tables etc, you can take a proper printout from a pdf file. You will need an Acrobat Reader though.)
Request a PDF file of this review by clicking here. (If your screen resolution can not be increased, or if printing this page is giving you problems like overlapping of graphics and/or tables etc, you can take a proper printout from a pdf file. You will need an Acrobat Reader though.)
 N.B. It is essential to read this journal - and especially this review as it contains several tables and high resolution graphics - under a screen resolution of 1600 x 1200 dpi or more. If the resolution is less than this, you may see broken or overlapping tables/graphics, graphics overlying text or other anomalies. It is strongly advised to switch over to this resolution to read this journal - and especially this review. These pages are viewed best in Netscape Navigator 4.7 and above.
N.B. It is essential to read this journal - and especially this review as it contains several tables and high resolution graphics - under a screen resolution of 1600 x 1200 dpi or more. If the resolution is less than this, you may see broken or overlapping tables/graphics, graphics overlying text or other anomalies. It is strongly advised to switch over to this resolution to read this journal - and especially this review. These pages are viewed best in Netscape Navigator 4.7 and above.
-Anil Aggrawal



 [ Major links ]
[ Major links ]
[ Aims and Objectives ] [ FAQ ] [ Editorial Board ] [ Contributing Partners ] [ Sitemap ]
[ Paper/Thesis submission guidelines ] [ Editorials - Cumulative Index ] [ Discussion ] [ Chat room ] [ Be our sponsor! ]
[ Cumulative index of Book Reviews sorted by | Publishers | General Interest Books | Technical Books ] [ Animated Reviews ] [ Featured Reviews ] [ E-books ]
[ Reviews with Quizzes ] [ Links ] [ Submit books/journals/software/multimedia for review ] [ journal CD ] [ History of the Journal ] [ Interviews ] [ Credits ]
[ Cumulative index of | Theses/dissertations | [ Online Courses ] [ Awards ] [ Anil Aggrawal's Internet Journal of Book Reviews - Sister Publication ]
[ Cumulative reviews of Software/Multimedia | Books on CD/Audio tapes ] | Calenders | Models ] [ contact us ]
[ Undergraduate section | Postgraduate section ] [ Forensic gadgets/toys/other tidbits ]

 Books for review must be submitted at the following address.
Books for review must be submitted at the following address.
 Professor Anil Aggrawal (Editor-in-Chief)
Professor Anil Aggrawal (Editor-in-Chief)
Anil Aggrawal's Internet Journal of Forensic Medicine and Toxicology
S-299 Greater Kailash-1
New Delhi-110048
India

 Click here to contact us.
Click here to contact us.
 This page has been constructed and maintained by Dr. Anil Aggrawal, Professor of Forensic Medicine, at the Maulana Azad Medical College, New Delhi-110002. You may want to give me the feedback to make this pages better. Please be kind enough to write your comments in the guestbook maintained above. These comments would help me make these pages better.
This page has been constructed and maintained by Dr. Anil Aggrawal, Professor of Forensic Medicine, at the Maulana Azad Medical College, New Delhi-110002. You may want to give me the feedback to make this pages better. Please be kind enough to write your comments in the guestbook maintained above. These comments would help me make these pages better.
 IMPORTANT NOTE: ALL PAPERS APPEARING IN THIS ONLINE JOURNAL ARE COPYRIGHTED BY "ANIL AGGRAWAL'S INTERNET JOURNAL OF FORENSIC MEDICINE AND TOXICOLOGY" AND MAY NOT BE REPOSTED, REPRINTED OR OTHERWISE USED IN ANY MANNER WITHOUT THE WRITTEN PERMISSION OF THE WEBMASTER
IMPORTANT NOTE: ALL PAPERS APPEARING IN THIS ONLINE JOURNAL ARE COPYRIGHTED BY "ANIL AGGRAWAL'S INTERNET JOURNAL OF FORENSIC MEDICINE AND TOXICOLOGY" AND MAY NOT BE REPOSTED, REPRINTED OR OTHERWISE USED IN ANY MANNER WITHOUT THE WRITTEN PERMISSION OF THE WEBMASTER
Questions or suggestions ? Please use ICQ 19727771 or email to dr_anil@hotmail.com
Page Professor Anil Aggrawal via ICQ


|
